Lecture Reports
Below you will find reports from our lectures. Either click the title to view the report online or download a copy by clicking on the file name next to 'Download report'. Use the search box on this page to find a particular report.
The talk presented to the Cirencester Science & Technology Society by Professor Harold Thimbleby, explaining the root cause of many of the problems with computer systems, and the action we should all take to rectify it.
- Category: Lecture Reports
- Date: Wednesday, 14 May 2025
- Professor Harold Thimbleby
- Swansea University
The talk presented to the Cirencester Science & Technology Society by Professor Lisa Methven, Programme Director for BSc Food Science, Sensory Science Centre, Reading University on the popular subject of the Chemistry of Chocolate.
- Category: Lecture Reports
- Date: Wednesday, 12 Mar 2025
- Professor Lisa Methven, Programme Director for BSc Food Science
- Sensory Science Centre, Reading University
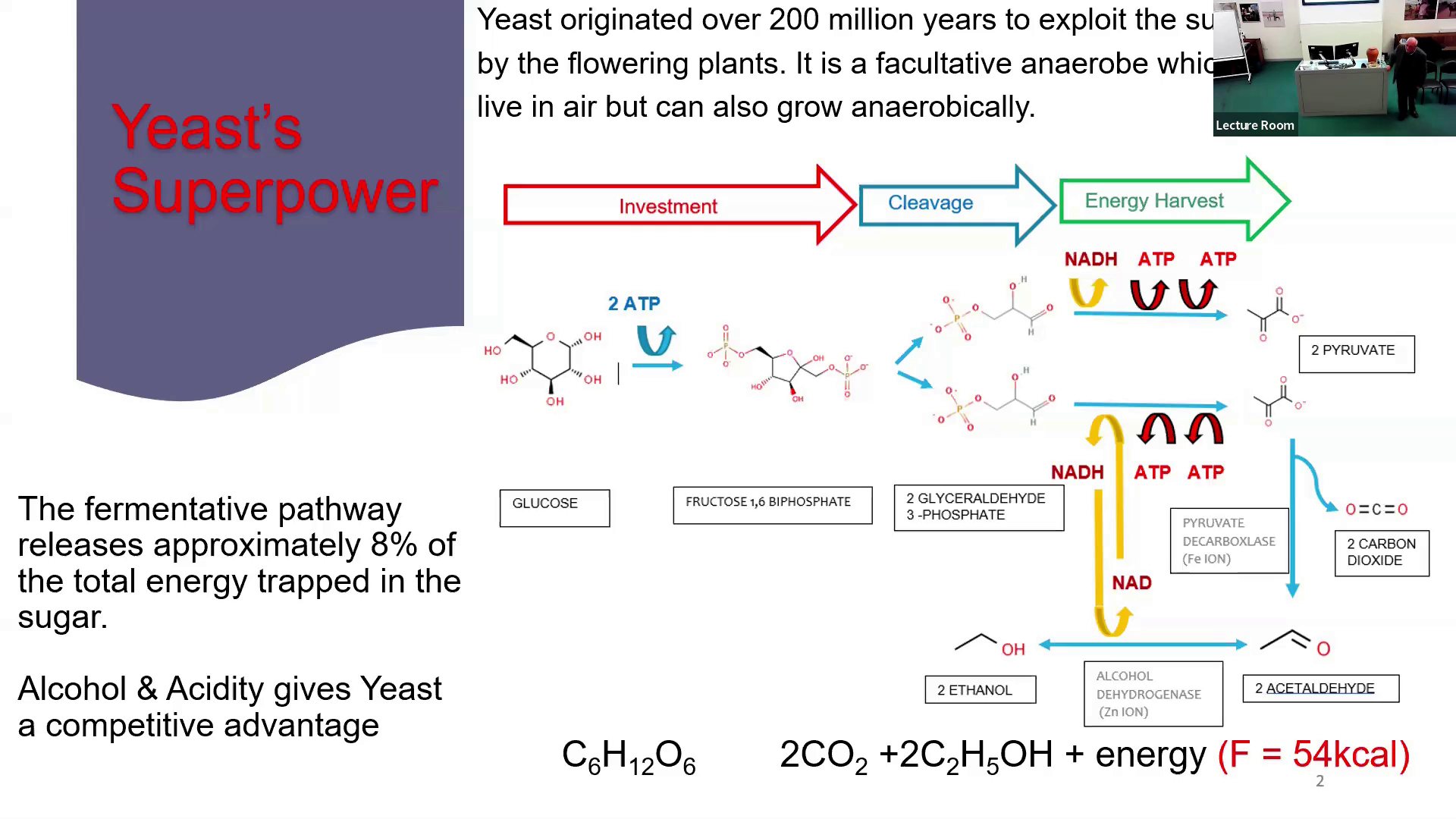
The presentation looks at how yeast has evolved and specialised in fermenting brewers wort, and the genetic and biochemical changes it has made to adapt to this new enviroment. It is the mainstay for a multi billion dollar fermentation industry around the world.
- Category: Lecture Reports
- Date: Wednesday, 12 Feb 2025
- Timothy O'Rourke BA
- The Brilliant Beer Co.
The talk presented to the Cirencester Science & Technology Society by Dr Alex Liu, Associate Professor Department of Earth Sciences, Cambridge University, introducing fossils of the enigmatic ‘Ediacaran biota’, which preserve our oldest records of early animal life, and explaining what we currently know about how and when animals diversified to ultimately dominate the planet.
- Category: Lecture Reports
- Date: Wednesday, 8 Jan 2025
- Dr Alex Liu
- Associate Professor, Department of Earth Sciences, Cambridge University